Cardiac emergencies rarely happen in ideal conditions. When an adult suddenly collapses and stops breathing normally, fast and coordinated action becomes critical. While one person can perform CPR alone, two trained responders working together can significantly improve the quality of care. This is why two-person CPR is a core skill taught in every BLS (Basic Life Support) course.
At Safety Training Seminars, two-person CPR training focuses on teamwork, communication, and efficiency. The goal is not just to teach steps, but to prepare responders to work together calmly under pressure. In this guide, you will learn how two-person CPR on an adult is performed in a BLS course and why this coordinated approach helps save lives.
Why Two-Person CPR Is Emphasized in BLS Training
Two-person CPR allows rescuers to share responsibilities, reduce fatigue, and maintain high-quality care for longer periods. In real emergencies—especially in workplaces, healthcare settings, or public spaces—multiple responders are often present. Knowing how to help together improves outcomes.
In a BLS course, students learn that effective CPR depends on consistent compressions, proper ventilation, and minimal interruptions. When one person works alone, fatigue can quickly reduce compression depth and rate. However, with two trained responders, tasks can be divided efficiently.
This teamwork approach strengthens First Aid and CPR response by ensuring continuous circulation and oxygen delivery. Ultimately, learning two-person CPR helps responders understand how to save a life more effectively through cooperation.
Recognizing When Two-Person CPR Is Needed
Before CPR begins, responders must quickly assess the situation. In BLS training, this assessment happens in seconds and sets the stage for coordinated care.
Two-person CPR is needed when:
- An adult is unresponsive
- The person is not breathing normally
- No signs of circulation are present
- A second trained responder is available
Once these conditions are confirmed, roles are assigned immediately. Clear role designation prevents confusion and delays. Quick recognition and teamwork allow care to begin without hesitation, which is critical in cardiac emergencies.
Assigning Roles in Two-Person CPR
Clear roles are the foundation of effective two-person CPR. In a BLS course, responders are taught to communicate clearly and assign responsibilities immediately.
Typically, roles include:
- Compressor: performs chest compressions
- Airway manager: delivers rescue breaths and monitors airway
- AED handler (if available): prepares and operates the device
Although only two people are required, roles may shift as the situation evolves. Communication ensures everyone knows their responsibility. This organization improves efficiency and reinforces how to help under stress.
How to Perform High-Quality Chest Compressions as a Team
Chest compressions are the most critical part of adult CPR. In two-person CPR, one rescuer focuses entirely on delivering consistent, effective compressions.
The compressor should:
- Place hands in the center of the chest
- Compress to an appropriate depth
- Maintain a steady rhythm
- Allow full chest recoil
- Minimize interruptions
Because fatigue affects compression quality, BLS courses teach rescuers to switch roles regularly. Switching every few minutes helps maintain effective compressions and prevents decline in performance. This teamwork directly improves how to save a life during prolonged resuscitation efforts.
Providing Rescue Breaths During Two-Person CPR
While one rescuer performs compressions, the second rescuer manages the airway and delivers breaths. This division of tasks improves ventilation efficiency and timing.
The airway rescuer should:
- Open the airway properly
- Deliver breaths at appropriate intervals
- Watch for visible chest rise
- Avoid excessive ventilation
Two-person CPR allows smoother transitions between compressions and breaths, reducing pauses. Effective ventilation ensures oxygen reaches the lungs while compressions circulate blood. Together, these actions support vital organs and reinforce the lifesaving power of CPR and BLS training.
Coordinating Compression-to-Breath Ratios
In a BLS course, responders practice maintaining proper timing between compressions and breaths. Coordination is key to avoiding unnecessary delays.
During two-person CPR:
- Compressions continue in steady cycles
- Breaths are delivered efficiently
- Communication signals when transitions occur
Verbal cues such as “switch” or “ready” help synchronize actions. This rhythm keeps care organized and effective. Good coordination helps responders stay calm and focused, even in high-stress environments.
Switching Roles Without Interrupting CPR
Role switching is essential to maintain high-quality CPR over time. However, interruptions must be minimized. BLS training teaches responders how to switch smoothly.
Best practices include:
- Communicating before switching
- Timing the switch during natural pauses
- Resuming compressions immediately
- Maintaining proper positioning
Smooth transitions reduce downtime and preserve circulation. This level of coordination demonstrates why two-person CPR is more effective than solo response when help is available.
Using an AED During Two-Person CPR
When an AED is available, one rescuer can continue CPR while the other prepares the device. This efficiency reduces interruptions and speeds care.
In two-person CPR:
- One rescuer continues compressions
- The other retrieves and prepares the AED
- Pads are applied quickly
- CPR resumes immediately after analysis or shock
This teamwork ensures the AED integrates smoothly into the response. Combining CPR, First Aid, and BLS skills creates a strong and effective emergency response.
What to Do If the Adult Shows Signs of Life
If the adult begins to breathe normally or shows signs of circulation, CPR should be paused and the situation reassessed. In BLS training, responders learn to transition care appropriately.
At this stage:
- Monitor breathing and responsiveness
- Keep the person comfortable
- Continue to observe until help arrives
Knowing when to stop CPR is just as important as knowing how to perform it. This awareness ensures care remains appropriate and responsive to changing conditions.
Common Mistakes Two-Person CPR Training Helps Prevent
Without training, multiple responders may unintentionally interfere with each other. BLS courses focus on preventing these common issues.
Mistakes include:
- Poor communication
- Delayed role switching
- Over-ventilation
- Long pauses during transitions
Training builds coordination and confidence. Practicing together allows responders to work as a unit rather than as individuals. This teamwork improves outcomes and reinforces how to help effectively.
Why Two-Person CPR Training Saves Lives
Two-person CPR maximizes efficiency, reduces fatigue, and improves care quality. These benefits directly increase the chance of survival during cardiac emergencies.
Learning two-person CPR through First Aid, CPR, and BLS education prepares individuals for real-world situations. Whether in a workplace, healthcare facility, or public space, trained responders can act together with confidence.
At Safety Training Seminars, BLS courses emphasize practical readiness. The goal is not just certification, but the ability to step forward and act when it matters most.
Turning Teamwork Into Lifesaving Action
Knowledge becomes lifesaving when responders trust their training and each other. Two-person CPR teaches cooperation, communication, and calm execution under pressure.
When responders work together effectively, they provide stronger, more consistent care. This teamwork transforms stressful moments into coordinated action—and that action saves lives.
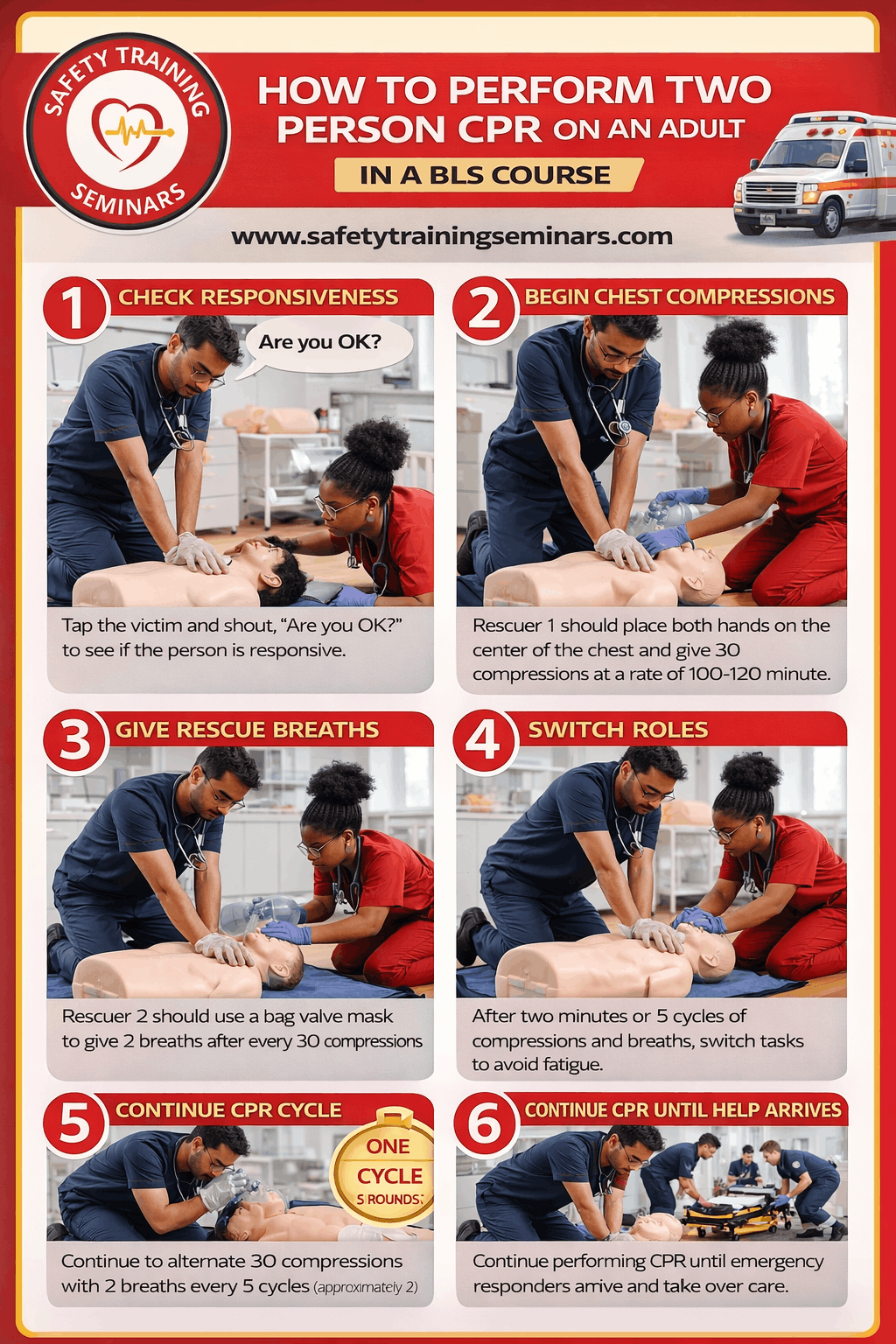
Final Thoughts: Preparedness Is a Shared Responsibility
Two-person CPR on an adult is a powerful example of how teamwork improves emergency response. Through BLS training, individuals learn how to act together with purpose and confidence.
Safety Training Seminars is committed to providing practical, accurate education that empowers people to help others in critical moments. When you know how to save a life—and how to do it together—you become part of a safer, more prepared community.